Naperville Integrated Wellness
NAPERVILLE'S TOP RATED LOCAL® FUNCTIONAL MEDICINE FACILITY
Irritable Bowel Syndrome (IBS) Treatment
We have all had temporary stomach upset and problems going to the bathroom, but for individuals suffering with irritable bowel syndrome (IBS) the discomfort and inconvenience can be disabling. Our IBS treatment center in Naperville is here to help with this digestion issue. IBS should not be confused with inflammatory bowel disease (IBD), which includes ulcerative colitis and Crohn’s disease; IBS is a common digestive tract disorder that affects the colon (large intestine) but does not cause damage to it. Naperville Integrated Wellness is your local functional treatment facility that specializes in treating IBS and other GI related health concerns. With a thorough health history, lab work and functional testing, we get to the root of the problem rather than just treat your symptoms. We get to know the whole YOU, not just your gastrointestinal system, and this allows us to uncover health issues that may be underlying your IBS symptoms. https://www.mayoclinic.org/diseases-conditions/irritable-bowel-syndrome/symptoms-causes/syc-20360016 Functional gastrointestinal disorders are characterized by chronic or recurring symptoms as a result of abnormal functioning of the GI (gastrointestinal) tract. This means normal function of the gut has been altered in some way. Syndrome means “running together.” IBS is a group of symptoms existing together. In the case of IBS, there are common symptoms (see below) but the cause of these symptoms or how they are related is not clearly understood. To summarize; IBS is a functional disorder (the gut is not working the way it should) and it is a syndrome (nobody knows exactly what causes it).The good news is that functional medicine doctors specializes in functional disorders and just because a single cause for IBS has not be identified, it does not mean it cannot be successfully treated. “IBS is a condition, in which the gut is hypersensitive and hyper-reactive to stimuli… This hyper-reactivity could be caused by increased mucosal permeability, increased numbers and/or responses of mast cells, and enhancement of nerve reflexes of the vagus nerve…” https://www.tandfonline.com/doi/abs/10.3109/00365528709090994 This means there can be gut permeability issues such as a leaky gut, changes in mast cells which would affect histamine levels in the gut and brain and altered function of the vagus nerve which is a large nerve that run from your brain to your gut. https://badgut.org/information-centre/a-z-digestive-topics/ibs-and-serotonin/ The Nervous System and IBS are not often seen to be connected, yet bowel function relies on the nervous system, more specifically the parasympathetic nervous system to function optimally. Proper nervous system function relies on proper nutrition, digestion, and absorption of nutrients. Communication between the gut and the nervous system relies on neurotransmitters, which are the method that nerves communicate with one another. Nerve signaling relies on proper nutrients and this brings us back to bowel function. “People with IBS often experience a strong urge to use the bathroom and may avoid going to places without easy access to one. This means that many everyday locations (malls, parks, places of worship, movie theaters, classrooms, offices) feel risky, and people might start to limit their activities as a result. People with IBS also start to fear and avoid many foods believed to trigger IBS attacks, often leading to loss of pleasure in eating as well as reduced opportunities to socialize.” Many individuals with IBS suffer from anxiety that may or may not be linked to the stressors listed above. The brain needs proper nutrition to function optimally. IBS and anxiety often occur together and can be related to poor dietary choices like those foods that contain high sugar and other simple carbohydrates, trans fats, caffeine, and alcohol. You see, the body needs certain foods to make neurotransmitters that are critical to brain function (more on this later). Even proper food choices may not be enough for proper brain function if you have IBS. Those individuals with IBS are often not digesting and absorbing enough of the nutrients needed for proper brain function. Still others with IBS are dealing with inefficient means of eliminating toxins and this can also affect brain function. Some of our patients with IBS are being treated with SSRIs or Selective Serotonin Reuptake Inhibitors. The most common symptoms of SSRI Irritable Bowel Syndrome are those who suffer with diarrhea (IBS-D) and this condition can be influenced or worsened by anxiety. This type of drug may or may not reduce symptoms of IBS-D. An important consideration is that this type of drug can create indigestion, anxiety, nausea, diarrhea or constipation (among other symptoms). Yes, that is correct, the drug can create NEW GI symptoms or worsen existing ones. Functional medicine helps with IBS syndrome and serotonin levels. We are able to assess serotonin levels via our functional testing, and this allows us to identify if supplemental support is necessary to help restore serotonin levels in the body. Since there are many causes for IBS, we want to identify and treat the source of the problem rather than treat a symptom and hope it will address the problem. “Most research has linked estrogen and progesterone with IBS. But scientists have also found that male sex hormones, like testosterone, may protect against the condition. This may be partly why men are less likely to get the disorder.” https://www.webmd.com/ibs/guide/hormones-ibs#1 Hormones, including stress hormones like cortisol, sex hormones like estrogen and progesterone, thyroid hormones, and gut hormones like serotonin, ghrelin, and peptide YY, all play roles in the development and management of irritable bowel syndrome (IBS). Fluctuations in these hormones can influence gastrointestinal motility, sensation, and secretion, potentially triggering or exacerbating IBS symptoms such as diarrhea, constipation, abdominal pain, and bloating. Additionally, the bidirectional communication between the brain and the gut, known as the brain-gut axis, is influenced by hormones and neurotransmitters, further impacting IBS symptomatology. Understanding these hormonal connections can aid in developing personalized treatment approaches for individuals with IBS. “Patients with IBS frequently experience worsening of their symptoms after eating. Moreover, a vast majority of IBS patients feel that distinct foods play pivotal role in triggering their symptoms. In a recent study, 58% of patients with IBS experienced GI symptoms from histamine-releasing food items such as milk, aged cheese, wine or beer.” http://www.jnmjournal.org/journal/view.html?doi=10.5056/jnm16203 Histamine is a not only a chemical of the immune system, but it also acts like a neurotransmitter and can significantly influence how the digestive system and the brain function. The relationship between irritable bowel syndrome (IBS) and histamine involves the potential role of histamine in triggering or exacerbating IBS symptoms, particularly in individuals with histamine intolerance or sensitivity. Histamine is a compound involved in the body’s immune response and is also found in certain foods, especially those that are aged, fermented, or high in histamine, as well as in some medications. In individuals with IBS, especially those with comorbid conditions like mast cell activation syndrome (MCAS) or histamine intolerance, high histamine levels in the gut may contribute to symptoms such as abdominal pain, bloating, diarrhea, and constipation. Histamine can affect gut motility, increase intestinal permeability, and stimulate the release of other mediators involved in inflammation and pain. Therefore, managing histamine levels through dietary modification, avoiding histamine-rich foods, and possibly using medications to reduce histamine release or block histamine receptors may help alleviate IBS symptoms in some individuals, particularly those with histamine intolerance. However, more research is needed to fully understand the role of histamine in IBS and to optimize management strategies for affected individuals. FODMAP = Fermentable Oligosaccharides, Disaccharides, Monosaccharides And Polyols…carbohydrates “Carbohydrate digestion and absorption is surprisingly complex. In order for carbohydrates to be properly digested, the wall (“brush border”) of your small intestine has to produce specific enzymes. If you do not optimally produce the enzymes or if the brush border of your small intestine is inflamed, carbohydrate digestion will be compromised.” The most popular diet plan for IBS would be the low FODMAP diet. The idea behind this is that the small intestine is not making sufficient enzymes to breakdown certain carbohydrates and this leads to the symptoms of IBS. I do not generally recommend this diet for my patients, not because I do not believe it has merit, but simply because it does not identify what caused the small intestine to become dysfunctional and lose the ability to breakdown these carbohydrates. Many things alter the health and function of the small intestine…food allergies, food sensitivities, stress, cortisol, bacteria, yeast, parasites, viruses, toxins, hormonal imbalances…etc. Food allergies and food intolerances are often one of the problems that results in IBS. Food allergies may be assessed by an allergy doctor. Many people have been to an allergy doctor to be treated for allergies. Some people have experienced success and many have not. Allergy doctors do not test for or address food sensitivities or intolerances. What that means is that if you have no allergies, there is no treatment. This is where functional medicine is able to help. Food intolerance is a symptom of an immune system problem that may be the result of leaky gut. To get resolution to food intolerance, we need to address the gut barrier and the immune system. Both allergies and food sensitivities need to be addressed and some foods (allergy foods) may have to be avoided altogether. Other food intolerances may be resolved over time and some amount of those foods may be incorporated back into the diet At Naperville Integrated Wellness, we create dietary programs that address food allergies and sensitivities. Our goal is to create a low inflammatory, gut-immune friendly plan that addresses your unique food responses. https://www.health.harvard.edu/blog/leaky-gut-what-is-it-and-what-does-it-mean-for-you-2017092212451 As previously mentioned in the section on food allergies and intolerances, I mentioned that this is an immune system problem. This problem is often a result of poor gut barrier function, otherwise known as leaky gut. Leaky gut can lead to poor bowel function, intestinal infections, autoimmunity and more. Long standing impaired bowel function is what gets diagnosed as a chronic IBS condition. Functional medicine recognizes and treats leaky gut. If the cause of your leaky gut is creating your IBS, then we are here to help. Conventional medicine does not even recognize leaky gut as a condition and therefore they provide no solution to this problem. At Naperville Integrated Wellness, we are looking for and addressing the cause of your IBS and healing the gut is an important part of that treatment. Learn more about leaky gut and IBS now. Functional medicine offers a comprehensive approach to addressing gastrointestinal conditions like small intestinal bacterial overgrowth (SIBO) and irritable bowel syndrome (IBS). It focuses on identifying and treating the root causes of these conditions rather than solely managing symptoms. In treating SIBO, practitioners may use testing to assess gut bacteria imbalances and implement dietary changes, probiotics, antimicrobial herbs or medications, and lifestyle modifications to rebalance the gut microbiota and address underlying issues like impaired gut motility or low stomach acid. Similarly, in IBS treatment, a personalized approach considers factors such as genetics, environment, lifestyle, and gut health, employing strategies such as dietary modifications, stress management techniques, targeted supplementation, and addressing gut dysbiosis or other imbalances. This holistic perspective emphasizes addressing underlying imbalances and interconnected body systems to promote optimal health, but it’s crucial to work with qualified healthcare professionals for safe and effective treatment. “Small intestinal bacterial overgrowth (SIBO) is a serious condition affecting the small intestine. It occurs when bacteria that normally grow in other parts of the gut start growing in the small intestine. That causes pain, gas, bloating and diarrhea (symptoms similar if not identical to IBS) It can also lead to malnutrition as the bacteria start to use up the body’s nutrients. https://www.healthline.com/health/sibo As you can see from the information above, there is not a single root cause for IBS. I’m guessing there will never be single cause identified, simply because many sufferers have been successfully treated using a variety of approaches. It is important to understand that IBS can have multiple causes. It can be caused by diet, a leaky gut, hormonal imbalances, nerve chemical imbalances, imbalances of digestive enzymes or stomach acid or nutrient deficiencies, etc. There is only one type of doctor that is familiar with all of these possible causes and that would be a functional medicine doctor. In our office we look for the underlying, root causes of IBS. We are able to accomplish this by consulting with you and collecting information through unique testing procedures that lead us to the root cause of your IBS. You are not alone, we are here to help. You want to feel like yourself again. You want your life back. Let’s see if we can get you there. Contact our IBS treatment center in Naperville today!IBS Treatment Center In Naperville
What Causes IBS in Naperville Residents?
 Muscle contractions in the intestine. The walls of the intestines are lined with layers of muscle that contract as they move food through your digestive tract. Contractions that are stronger and last longer than normal can cause gas, bloating and diarrhea. Weak intestinal contractions can slow food passage and lead to hard, dry stools.
Muscle contractions in the intestine. The walls of the intestines are lined with layers of muscle that contract as they move food through your digestive tract. Contractions that are stronger and last longer than normal can cause gas, bloating and diarrhea. Weak intestinal contractions can slow food passage and lead to hard, dry stools.
A “functional” gastrointestinal disorder and “syndrome.”
Nervous system
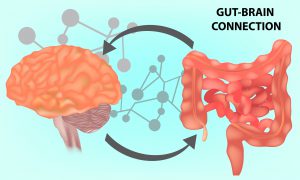 “The altered bowel function, abdominal pain, and sensitivity symptoms indicative of IBS result from what appears to be a disturbance in the interaction among the gut, the brain, and the Autonomic Nervous System – which includes the Parasympathetic (vagus nerve) Sympathetic, and the Enteric Nervous System – or ENS – now recognized as the “brain below.” The ENS is also called the “second brain” of your body.
“The altered bowel function, abdominal pain, and sensitivity symptoms indicative of IBS result from what appears to be a disturbance in the interaction among the gut, the brain, and the Autonomic Nervous System – which includes the Parasympathetic (vagus nerve) Sympathetic, and the Enteric Nervous System – or ENS – now recognized as the “brain below.” The ENS is also called the “second brain” of your body. Nervous system and IBS Connection
Anxiety
IBS and Anxiety Connection
What is the Role of Serotonin and IBS
 Scientific evidence strongly suggests that serotonin ibs is one of the most important signaling molecules (nerve chemical) involved in gut function – and that alterations in serotonin signaling may contribute to IBS symptoms. Ninety-five percent of the serotonin found in the body resides in the gut. Altered serotonin ibs the gut can contribute to IBS and altered serotonin balance in the brain can lead to anxiety, problems with sleep or depression.
Scientific evidence strongly suggests that serotonin ibs is one of the most important signaling molecules (nerve chemical) involved in gut function – and that alterations in serotonin signaling may contribute to IBS symptoms. Ninety-five percent of the serotonin found in the body resides in the gut. Altered serotonin ibs the gut can contribute to IBS and altered serotonin balance in the brain can lead to anxiety, problems with sleep or depression. How do SSRI’s Affect IBS?
Hormones
Interweaving Hormones and IBS
Histamine
IBS and Histamine Relationship
Food allergies, Food intolerance and Low FODMAP
Food Allergies, Food Intolerances and the IBS Connection
Leaky Gut
 “Inside our bellies, we have an extensive intestinal lining covering more than 4,000 square feet of surface area. When working properly, it forms a tight barrier that controls what gets absorbed into the bloodstream. An unhealthy gut lining may have large cracks or holes, allowing partially digested food, toxins, and bugs to penetrate the tissues beneath it. This may trigger inflammation and changes in the gut flora (gut microorganisms) that could lead to problems within the digestive tract and beyond.” A leaky gut can cause IBS as well as many other health problems.
“Inside our bellies, we have an extensive intestinal lining covering more than 4,000 square feet of surface area. When working properly, it forms a tight barrier that controls what gets absorbed into the bloodstream. An unhealthy gut lining may have large cracks or holes, allowing partially digested food, toxins, and bugs to penetrate the tissues beneath it. This may trigger inflammation and changes in the gut flora (gut microorganisms) that could lead to problems within the digestive tract and beyond.” A leaky gut can cause IBS as well as many other health problems. Leaky Gut and IBS Connection
SIBO = Small Intestinal Bacterial Overgrowth
What is SIBO?

Schedule An IBS Treatment Center Appointment In Naperville
CONTACT
Call: (630) 210-8391 or fill out the form below
"*" indicates required fields
