Naperville Integrated Wellness
NAPERVILLE'S TOP RATED LOCAL® FUNCTIONAL MEDICINE FACILITY
New Migraine Treatment
A Natural Solutions To Migraines with Functional Medicine
We have a new approach to treating migraines, and we are getting great results with it. No, it is not a new drug, dietary supplement or plant recently discovered in a remote part of the world. What we do is address the root causes of dysfunction in the body that result in migraines. Did you know? Serotonin and migraines have a strong connection? Learn more now. If you suffer from migraines, you have probably gone to your primary care physician or maybe even a neurologist and received medication. However, most medications used for migraines address only one possible cause. Medications like Triptans, are a group of drugs that alter how serotonin works in your body; drugs like Imitrex, Relpax and Zomig. A new group of drugs called CGRP antagonists include Aimovig and Ajovy. These drugs primarily affect the nerves. These drugs are believed to block chemical normal nerve activity so that pain signals from the nerves are reduced. In a nutshell, they are an advanced painkiller. Later in this article I will discuss the “migraine nerve” that is responsible for the pain you experience with a migraine. Other drugs may include beta-blockers, antidepressants, anti-inflammatory drugs, antihistamines, etc. As a functional medicine doctor, I look for root causes of health problems. I have found that that there are 3 major factors involved when treating migraines. In this article I will cover the 3 main migraine generators. We will even go one step further and see how they all affect one another. So, there is not a single cause for migraines. If there were, then we would only need one drug and it would work for all migraine sufferers. Let’s start with how a migraine occurs… A functional medicine appointment with a Natural Migraine Specialist near Chicago provides a comprehensive and tailored approach to addressing your migraines. The process begins with an in-depth consultation, exploring your medical history, lifestyle, and any potential triggers that may be contributing to your condition. Advanced diagnostic tests may be used to uncover imbalances in areas such as hormones, nutrition, gut health, or inflammation. With this information, the specialist will develop a personalized care plan focused on natural methods to reduce migraine frequency and intensity. From dietary recommendations to stress management techniques and targeted supplements, the approach prioritizes long-term relief by addressing the root causes of your migraines. Migraines can stem from a variety of root causes, many of which are interconnected and unique to each individual. Hormonal imbalances, particularly fluctuations in estrogen, are a common trigger, especially in women. Nutritional deficiencies, such as low magnesium or vitamin D levels, can also play a significant role in triggering migraines. Gut health issues, including food sensitivities or imbalances in the microbiome, may contribute to systemic inflammation, which is often linked to chronic headaches. Environmental factors, such as exposure to toxins or allergens, can also provoke migraines in susceptible individuals. Additionally, stress and poor sleep patterns are known to disrupt brain chemistry, potentially leading to episodes. Identifying these underlying causes through a functional medicine approach allows for targeted interventions that address the specific triggers affecting each person. By focusing on these root causes, a Natural Migraine Specialist near Chicago can provide relief and help prevent future migraines. Older theories about migraines suggested that symptoms were possibly due to fluctuations in blood flow to the brain. Now many headache doctors and researches realize that changes in blood flow and blood vessels don’t initiate the pain, but contribute to it. Today, it is widely understood that chemical compounds and hormones, such as serotonin and estrogen, often play a role in pain sensitivity for migraine sufferers. When serotonin or estrogen levels change, the result for some is a migraine. Serotonin levels may affect both sexes, while fluctuating estrogen levels affect women only. https://www.hopkinsmedicine.org/health/conditions-and-diseases/headache/how-a-migraine-happens These 3 natural and beneficial chemicals are most commonly involved in migraines. You can’t alter one of these chemicals without affecting the others and the end result is that it triggers a very important nerve. I call this the “migraine nerve” and it is responsible for pain you experience with a migraine. “Migraine is a predominantly female disorder. Menarche, menstruation, pregnancy, and menopause, and also the use of hormonal contraceptives and hormone replacement treatment may influence migraine occurrence. Migraine usually starts after menarche, occurs more frequently in the days just before or during menstruation, and ameliorates during pregnancy and menopause. Those variations are mediated by fluctuation of estrogen levels through their influence on cellular excitability or cerebral vasculature.” The Journal of Headache and Pain https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3311830/ “Biochemical evidence suggests central and peripheral roles for estrogen in the pathophysiology of menstrual migraine, and interactions with serotonergic (serotonin) components.” This means estrogen itself is involved in the cause of migraines but it also affects how serotonin works, which will also contribute to migraines. Journal of the American Medical Association https://jamanetwork.com/journals/jama/fullarticle/202685 Serotonin is a chemical that affects our blood vessels, our mood and how we perceive pain. Serotonin migraines can cause blood vessels to contract or relax. A common medication used to manage migraines is Imitrex and it binds to specific serotonin receptors that cause the blood vessels in your head to constrict. “Sumatriptan (Imitrex) binds strongly to serotonin 5-HT1B/1D receptors and is thought to relieve migraine symptoms through an inhibition of pro-inflammatory substances and a constriction of cranial blood vessels.” This demonstrates the importance of proper balance and function in the body. It helps regulate blood vessels and reduces inflammation. So what can we say about serotonin and migraines? They are connected. https://www.drugs.com/tips/sumatriptan-patient-tips Serotonin headaches, often referred to as serotonin migraines, are believed to result from fluctuations in serotonin levels—a neurotransmitter integral to mood regulation, vascular function, and pain perception. While medications can offer relief, many individuals seek natural approaches to manage and prevent these headaches. In summary: Natural healing for serotonin migraines focuses on restoring neurotransmitter balance, calming inflammation, and supporting the body’s stress and detox pathways. Personalization is key—what works for one person may trigger another. Migraine headache location can offer important clues about underlying triggers and mechanisms. Common migraine headache locations include one side of the head (unilateral), behind the eyes, or in the temples, though they can also present as throbbing pain in the forehead or the back of the head. The specific migraine headache location may relate to vascular changes, nerve irritation, or muscular tension. For example, migraines that begin around the eyes may be linked to sinus pressure or ocular strain, while those affecting the neck and occiput can suggest cervicogenic involvement. A serotonin headache location is often less specific but can manifest similarly, especially when serotonin imbalance causes widespread vasodilation or neural hypersensitivity. These headaches may be triggered by rapid serotonin level changes due to medications, hormonal shifts, or stress, and their location may shift depending on the individual’s sensitivity patterns. Understanding location helps tailor treatment and identify contributing factors such as posture, hormone cycles, or dietary triggers. The nerve that carries the pain signals of a migraine is called the trigeminal nerve. You have 2 of these nerves, one from the left side Estrogen and serotonin play a significant role in migraines. The trigeminal nerve carries the pain signals from the affected blood vessels to the rest of your brain and that is how you experience or feel the pain of the migraine. So, I am calling the trigeminal nerve the “migraine nerve.” You could not experience pain from a migraine without this nerve. This nerve has receptors for estrogen and serotonin…meaning they influence how this nerve works and how you feel the pain of a migraine. “Estrogen acts as a neurosteroid influencing the pain pathway associated with migraine by binding to its receptors (estrogen receptors) present on the trigeminal nerves. The trigeminovascular system consists of a network of cranial blood vessels and their trigeminal innervations that convey the pain information to the central nervous system where migraine pain is perceived. Decreased levels of a neurotransmitter serotonin, are also linked to migraine. The implication of serotonin in migraine has been indicated by studies showing the presence of its receptors (5-HT receptors) on the trigeminal nerve and cranial vessels and also by the relief obtained after serotonin administration.” Annals of Neurosciences https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4117063/ “Histamine has been known to cause a vascular type headache (migraine) for almost a hundred years.” The Journal of Headache and Pain https://thejournalofheadacheandpain.biomedcentral.com/articles/10.1186/s10194-019-0984-1 “Histamine-induced headache is a vascular (blood vessel) headache. In migraine patients, plasma histamine concentrations have been shown to be elevated both during headache attacks and during symptom-free periods.” The American Journal of Clinical Nutrition Histamine is the chemical that causes the symptoms associated with allergies…itchy eyes, runny nose, etc. but that is only one of many functions of histamine in your body. It is a chemical that is involved in the function of the immune system, but it also acts as a There are histamine receptors in blood vessels, the brain and nerves that carry pain signals. Histamine will increase pain signals while serotonin tends to decrease pain signals in the body. “The pain caused by the trigeminal nerve has been described as the most agonizing known to humankind…” https://www.theguardian.com/lifeandstyle/2011/oct/17/mapping-the-body-trigeminal-nerve If you do not make enough of the enzyme (DAO) to breakdown excess histamine in your body, you may experience a migraine. The health of your digestive system will also influence your ability to breakdown histamine, the preventing a migraine. H1 receptors are found in smooth muscles, blood vessels, and the central nervous system, playing a central role in allergic and inflammatory responses. They contribute to symptoms like itching, swelling, sneezing, and bronchoconstriction, and also influence sleep-wake regulation in the brain. Because of their widespread effects, H1 receptors are a common target for antihistamine medications such as diphenhydramine, which are used to manage allergies, motion sickness, and sleep disturbances. These receptors are found in smooth muscles, vascular endothelium, central nervous system (CNS), and peripheral tissues. H1 Receptors mediate allergic and inflammatory responses. They cause vasodilation, increased vascular permeability (leading to swelling and hives), and smooth muscle contraction (e.g., in the bronchi). They also play a role in wakefulness and sleep regulation in the central nervous system Overactivation leads to symptoms of allergic reactions such as itching, sneezing, and asthma. Antihistamine medications that target H1 receptors include diphenhydramine and are used for allergies, motion sickness, and insomnia. These receptors are predominantly found in the stomach’s parietal cells, heart, and some immune cells. H2 receptors stimulate the secretion of gastric acid, modulate heart rate and contraction strength and are involved in immune regulation and inflammation. Overactivation can cause acid-related gastrointestinal conditions such as ulcers and gastroesophageal reflux disease (GERD). Medications that target H2 receptors include ranitidine & famotidine and are used to treat peptic ulcers and acid reflux. These receptors are primarily found in the CNS and peripheral nervous system. They act as an auto receptor to regulate histamine synthesis and release. They also modulate the release of other neurotransmitters such as dopamine, acetylcholine, and norepinephrine. They also play a part in sleep-wake cycles, cognition, and appetite regulation. Dysregulation may contribute to neurological conditions like Alzheimer’s disease, schizophrenia, and narcolepsy. H3 receptor medications are being explored for cognitive disorders and sleep-related issues. These receptors are found in the bone marrow, white blood cells (e.g., eosinophils, mast cells), and the gastrointestinal tract. They play a role in immune response and chemotaxis (movement of immune cells). They also modulate inflammation and allergic responses. Associated with chronic inflammatory diseases, autoimmune disorders, and pruritus (itching). H4 receptor medications are being investigated for conditions like asthma, rheumatoid arthritis, and atopic dermatitis. As you have just read, health issues relating to histamine activity in the body can be numerous and sometimes difficult to identify. Functional medicine aims to isolate and treat the root cause of your symptoms. Histamine symptoms are often triggered by foods and a functional medicine treatment will consider food triggers in prescribing a low inflammatory gut-immune friendly food plan. In addition to avoiding food triggers, it is important to know if you do not make enough of the enzyme (DAO) to breakdown excess histamine in your body. This could be the reason you experience a migraine (or another symptom). The health of your digestive system will also influence your ability to breakdown histamine, this could be critical in preventing a migraine. Whether your histamine response causes you to experience a migraine or some other symptom, you can expect a thorough histamine intolerance consultation here in Naperville at Naperville Integrated Wellness. The 5 C’s of Migraines refer to five common triggers that often contribute to migraine development. Each “C” represents a category that influences brain sensitivity, vascular tone, and neurotransmitter balance—especially serotonin and histamine levels. Understanding these can help identify patterns and support natural migraine prevention. Many of the foods listed as “migraine triggers” are foods and drinks that are high in histamine or cause your body to release too much histamine, triggering a migraine. Other foods listed as “migraine triggers” include red wine and foods containing yeast. Aged cheese is often considered one of the worst offenders due to its tyramine content, especially when combined with other triggers like stress or hormonal shifts. However, cured meats with MSG or nitrates are also top culprits in many cases. In our office we often discover that migraine sufferers have some degree of histamine intolerance. This means they have difficulty breaking down excess histamine. This is how diet can play a significant role in the treatment of migraines. “Hence, histamine release and accumulation in the trigeminal nerve plays an important role in the pathogenesis (cause) of neuralgia (nerve pain). Food triggers migraines by affecting the nervous system, vascular system, and neurotransmitter balance—especially serotonin and histamine. In susceptible individuals, certain foods can lead to vasodilation, inflammatory responses, or neuronal hyperexcitability, all of which contribute to the onset of a migraine. Additionally, poor detoxification pathways (like impaired MAO or DAO enzyme activity) can lead to the buildup of food-derived amines and histamines, intensifying the body’s reaction. In our office we often discover that migraine sufferers have some degree of histamine intolerance. This means they have difficulty breaking down excess histamine. This is how diet can play a significant role in the treatment of migraines. “Hence, histamine release and accumulation in the trigeminal nerve plays an important role in the pathogenesis (cause) of neuralgia (nerve pain). Journal of Oral and Maxillofacial Research When the 3 factors leading to a migraine are assessed and addressed, most of our patients who suffer with migraines experience significant improvement or the elimination of migraines entirely. There is no medication that addresses these 3 causes. Some address serotonin, some address the pain, some address inflammation, some address how blood vessels work, etc. In functional medicine we look for the root cause of migraines. As you now see, it can be due to various chemical imbalances. Each of these 3 main factors are medically recognized causes of migraines, but they are not being addressed nor or doctors recognizing how all estrogen, serotonin and histamine all influence each other. So what makes our Serotonin and Migraines treatment new is that we are not just focusing on a single cause, nor are we trying to suppress the results of these causes (like inflammation). We are addressing the root cause of migraines so that our patients can have far fewer migraines, less debilitating migraines and many cases, no migraines at all. We are achieving this without the use of drugs and most of our patients are able to reduce or eliminate the migraine medications they were taking. If you’re seeking a migraine specialist in Naperville, Naperville Integrated Wellness offers a unique and comprehensive approach to headache relief through the lens of functional medicine. As a trusted Naperville migraine specialist, our clinic focuses on identifying and addressing the root causes of migraines, rather than simply masking symptoms. Whether your headaches are linked to hormonal shifts, food sensitivities, neurotransmitter imbalances, or inflammation, we provide personalized migraine solutions with functional medicine to help restore balance and prevent future attacks. If you’re ready to take a deeper look at your health and finally get lasting relief, connect with a dedicated migraine specialist in Naperville at Naperville Integrated Wellness. Contact us today! Aggarwal, M., Puri, V., & Puri, S. (2012). Effects of estrogen on the serotonergic system and calcitonin gene-related peptide in trigeminal ganglia of rats. Annals of Neurosciences, 19(4), 151-157. Retrieved 10 23, 2020, from https://ncbi.nlm.nih.gov/pmc/articles/pmc4117063 Brandes, J. L. (2006). The Influence of Estrogen on Migraine: A Systematic Review. JAMA, 295(15), 1824-1830. Retrieved 10 23, 2020, from https://jamanetwork.com/journals/jama/fullarticle/202685 Chai, N. C., Peterlin, B. L., & Calhoun, A. H. (2014). Migraine and estrogen. Current Opinion in Neurology, 27(3), 315-324. Retrieved 10 23, 2020, from https://ncbi.nlm.nih.gov/pmc/articles/pmc4102139 Maintz, L., & Novak, N. (2007). Histamine and histamine intolerance. The American Journal of Clinical Nutrition, 85(5), 1185-1196. Retrieved 10 23, 2020, from https://academic.oup.com/ajcn/article/85/5/1185/4633007 Sacco, S., Ricci, S., Degan, D., & Carolei, A. (2012). Migraine in women: the role of hormones and their impact on vascular diseases. Journal of Headache and Pain, 13(3), 177-189. Retrieved 10 23, 2020, from https://ncbi.nlm.nih.gov/pmc/articles/pmc3311830Natural Migraine Specialist near Chicago
Root Cause of Migraines
How a Migraine Happens…
3 chemicals that cause migraines
Estrogen—Serotonin—Histamine
“migraine nerve”
Estrogen
 Why more women get migraines than men…
Why more women get migraines than men…Estrogen alters how serotonin and histamine work in your body…
 Serotonin and migraines…
Serotonin and migraines…Healing Serotonin Headaches Naturally
Dietary Strategies and Choices:
Incorporate Key Nutrients to Support neurotransmitter Balance:
Regular Exercise:
Sunlight Exposure:
Sleep Hygiene:
Stress Management:
Detoxification and Environmental Support
Migraine Headache Location: Meaning and Causes
Why you feel pain…
“migraine nerve”
 of your brainstem and one from the right.
of your brainstem and one from the right. Histamine
 neurotransmitter (serotonin is also a neurotransmitter).
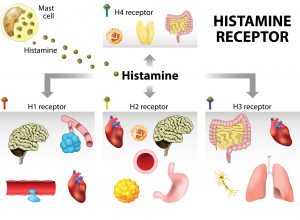
neurotransmitter (serotonin is also a neurotransmitter). Types of Functions of Histamine Receptors
H1 Receptors
H2 Receptors
H3 Receptors
H4 Receptors
How to Naturally Flush Histamine from the Body
The 5 C’s of Migraines
Worst Food for Migraines
Why Does Food Trigger Migraines?
Contact Our Migraine Specialist in Naperville
CONTACT
Call: (630) 210-8391 or fill out the form below
"*" indicates required fields
