Naperville Integrated Wellness
NAPERVILLE'S TOP RATED LOCAL® FUNCTIONAL MEDICINE FACILITY

IBS and Functional Medicine
As a leading Chicago functional medicine doctor, I see patients every day that suffer with chronic digestion issues. Our Naperville functional medicine specialist is here to help get to the root of your chronic condition. IBS or irritable bowel syndrome is one of the most common problems we see in our Chicago-based office.
This article will look at IBS from a conventional and functional medicine perspective. Hopefully this will provide you with a greater understanding of this condition.
“Irritable bowel syndrome (IBS) is a common disorder that affects the large intestine. Signs and symptoms include cramping, abdominal pain, bloating, gas, and diarrhea or constipation, or both.”
https://www.mayoclinic.org/diseases-conditions/irritable-bowel-syndrome/symptoms-causes/syc-20360016
What is IBS? A functional bowel disorder…
IBS is a functional bowel disorder. This basically means that there is no single cause, and it is not diagnosed by testing. This means we don’t diagnose IBS and other functional bowel disorders based on a type of blood test, stool test or another medical test. Functional bowel disorders are diagnosed based on your symptoms.
Since IBS is a “functional” problem, it makes sense that applying a functional medicine approach makes the most sense.
Medical Definition
“IBS is a functional bowel disorder in which abdominal pain or discomfort is associated with defecation or a change in bowel habit, and with features of disordered defecation. The functional bowel disorders are identified only by symptoms. Therefore, a symptom-based classification is necessary for clinical diagnosis, evidence-based management, and research.
 Functional Bowel Disorders
Functional Bowel Disorders
Functional bowel disorders are functional gastrointestinal disorders with symptoms attributable to the middle or lower gastrointestinal tract. These include the IBS, functional bloating, functional constipation, functional diarrhea, and unspecified functional bowel disorder.
Throughout the world, about 10%–20% of adults and adolescents have symptoms consistent with IBS, and most studies find a female predominance.”
https://www.gastrojournal.org/article/S0016-5085(06)00512-9/fulltext
Another important feature about functional bowel disorders is that traditional testing like endoscopies and colonoscopies yields no information for identifying IBS. You are often told that you are fine, and nothing was found during the testing. This means your symptoms are not the result of an identifiable pathology (disease process) in the anatomy of the gastrointestinal system. This is good news! BUT, if you do not know about functional medicine, you leave your doctor’s office feeling worse because you still have seemingly no identifiable cause for your symptoms!
Functional Medicine and IBS
Because IBS is a functional disorder, it is most effectively treated with functional medicine. A conventional approach to treating IBS will address the predominant symptom(s) associated with the condition, namely diarrhea or constipation. A functional medicine approach will look for and treat what is found to be the cause. These potential causes will be discussed further in the following paragraphs.
What causes IBS?
The precise cause of IBS isn’t known. Factors that appear to play a role include:
Muscle contractions in the intestine
The walls of the intestines are lined with layers of muscle that contract as they move food through your digestive tract. Contractions that are stronger and last longer than normal can cause gas, bloating and diarrhea. Weak intestinal contractions can slow food passage and lead to hard, dry stools. (Note: your nervous system controls these muscle contractions).
Nervous system
Abnormalities in the nerves in your digestive system may cause you to experience greater than normal discomfort when your abdomen stretches from gas or stool. Poorly coordinated signals between the brain and the intestines can cause your body to overreact to changes that normally occur in the digestive process, resulting in pain, diarrhea, or constipation.
Infection
IBS can develop after a severe bout of diarrhea (gastroenteritis) caused by bacteria or a virus. IBS might also be associated with a surplus of bacteria in the intestines (bacterial overgrowth). The most common location for this type of overgrowth is the small intestine and we call this SIBO; Small Intestinal Bacterial Overgrowth.

Early life stress
People exposed to stressful events, especially in childhood, tend to have more symptoms of IBS. This would ultimately have a negative impact on the nervous system; and more specifically what we call the autonomic nervous system which controls bodily functions that are necessary not only for the body to remain alive but to function properly.
Changes in gut microbes
Examples include changes in bacteria, fungi and viruses, which normally reside in the intestines and play a key role in health. Research indicates that the microbes in people with IBS might differ from those in healthy people.
Functional Medicine Approach to IBS
IBS has many potential causes, as mentioned above. It is the job of a functional medicine approach is to identify the underlying factors and create a treatment plan to restore proper function. A functional medicine approach to IBS is quite different than a conventional approach in 2 distinct ways. Conventional medicine looks to 1. create a diagnosis that explains the symptoms, and 2. prescribe a medication to treat the symptoms caused by the diagnosed condition. One the other hand, a functional medicine doctor 1. evaluates the symptoms presented by looking at the factors that may have led to the creation of the symptoms. This is done by identifying the dysfunction in the system(s) in the body that may underly the symptoms. Then a functional medicine IBS specialist will 2. create a treatment plan for the patient. The patient must then follow the treatment plan over the period of time recommended by the doctor.
Another important element for a successful functional medicine IBS treatment involves follow up appointments to measure the outcomes of the IBS treatment. Modifications or additional steps may be necessary over the course of time to ensure successful outcomes. This approach, and the results achieved, are based on a collaborative effort on the part of the IBS specialist and the patient. Without this important step, important considerations of the IBS treatment may be missed, and results may be less than optimal.
Common Triggers For IBS
Symptoms of IBS can be triggered by food and stress:
- Food. The role of food allergy or intolerance in IBS isn’t fully understood. Many people have worse IBS symptoms when they eat or drink certain foods or beverages, including wheat, dairy products, citrus fruits, beans, cabbage and milk.
I have found various foods to contribute significantly to IBS. The reason for this typically falls into two major categories.
- Immune system reactions to foods.
- Difficulty digesting certain foods.
Immune system reactions to foods:
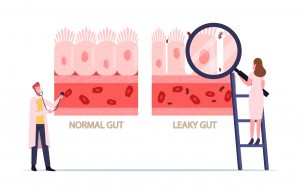 I evaluate food and immune system reactions using food sensitivity and allergy testing. This is a blood test, and we measure what are called antibodies. Your immune system makes antibodies to what it considers to be an “enemy” to your body. We have unique methods of how we interpret the results of this kind of testing because not all immune responses to food will result in the production of antibodies. A leaky gut is often found in individuals with food sensitivities or food allergies. Leaky gut occurs in your small intestine and often occurs in functional bowel disorders like IBS.
I evaluate food and immune system reactions using food sensitivity and allergy testing. This is a blood test, and we measure what are called antibodies. Your immune system makes antibodies to what it considers to be an “enemy” to your body. We have unique methods of how we interpret the results of this kind of testing because not all immune responses to food will result in the production of antibodies. A leaky gut is often found in individuals with food sensitivities or food allergies. Leaky gut occurs in your small intestine and often occurs in functional bowel disorders like IBS.
Difficulty Digesting Certain Foods:
Probably the most recommended diet for IBS patients by their primary care physician or gastroenterologist is the low FODMAP diet.
“FODMAPs or fermentable oligosaccharides, disaccharides, monosaccharides, and polyols are short chain carbohydrates that are poorly absorbed in the small intestine and are prone to absorb water and ferment in the colon.”
https://en.wikipedia.org/wiki/FODMAP
This is not an immune-system-based diet; it is a diet based on poor digestion of certain carbohydrates. I find that most patients with this problem also have food sensitivities and or a leaky gut. This occurs in the small intestine. Your pancreas makes digestive enzymes, but so does your small intestine. Your small intestine is the portion of your digestive tract where you absorb the food and nutrients you have consumed.
“Carbohydrate digestion and absorption is surprisingly complex. In order for carbohydrates to be properly digested, the wall (“brush border”) of your small intestine has to produce specific enzymes. If you do not optimally produce the enzymes or if the brush border of your small intestine is inflamed, carbohydrate digestion will be compromised.”
Stress as a trigger:
- Stress. Most people with IBS experience worse or more-frequent signs and symptoms during periods of increased stress.
https://www.mayoclinic.org/diseases-conditions/irritable-bowel-syndrome/symptoms-causes/syc-20360016
Stress affects the nervous system and results in increased production of stress hormones/chemicals. These same chemicals can have a negative impact on how the digestive system and the immune system function.
Medications specifically for IBS
 I have provided a list of medications primarily for you to see that they are directed at gut function and most of them ultimately are overriding the nervous system in some way. Either by affecting how the muscles of the bowel are working, how the contents of the bowel are moved along, or regulating fluid content of the stool; etc. These functions are normally achieved through healthy neurological function of the gut.
I have provided a list of medications primarily for you to see that they are directed at gut function and most of them ultimately are overriding the nervous system in some way. Either by affecting how the muscles of the bowel are working, how the contents of the bowel are moved along, or regulating fluid content of the stool; etc. These functions are normally achieved through healthy neurological function of the gut.
I have found IBS to be mainly caused by altered function of the nervous system and immune system. Most of your body’s immune system is in and around your digestive system by the by way. So, I often find the immune system and the nervous system both playing a role in IBS and other functional bowel disorders.
Sometimes hormones play a role in the frequency and severity of IBS symptoms, but I don’t consider them to be the root cause. I believe they alter the intensity of dysfunction that is already present within the nervous system and immune system.
Medications approved for certain people with IBS include:
Alosetron, eluxadoline, rifaximin, lubiprostone, and linaclotide are medications for IBS that either relax the colon, reduce diarrhea, treat bacterial overgrowth, or increase intestinal fluid secretion, with specific approvals for severe cases and certain populations.
Alosetron (Lotronex)
Alosetron is designed to relax the colon and slow the movement of waste through the lower bowel. It has been linked to rare but important side effects, so it should only be considered when other treatments aren’t successful.
Eluxadoline (Viberzi)
Eluxadoline can ease diarrhea by reducing muscle contractions and fluid secretion in the intestine and increasing muscle tone in the rectum. Eluxadoline has also been associated with pancreatitis, which can be serious and more common in certain individuals.
Rifaximin (Xifaxan)
This antibiotic can decrease bacterial overgrowth and diarrhea. This medication is often used as treatment for another bowel disorder called SIBO or Small Intestinal Bacterial Overgrowth.
Lubiprostone (Amitiza)
Lubiprostone can increase fluid secretion in your small intestine to help with the passage of stool. It’s approved for women who have IBS with constipation and is generally prescribed only for women with severe symptoms that haven’t responded to other treatments.
Linaclotide (Linzess)
Linaclotide also can increase fluid secretion in your small intestine to help you pass stool.
Other medications used in the management of IBS:
Options for IBS management encompass fiber supplements for constipation, laxatives if fiber fails, anti-diarrheal medications or bile acid binders, anticholinergic medications for bowel spasms, and antidepressants like tricyclics or SSRIs for pain and depression.
Fiber supplements
Taking a supplement such as psyllium (Metamucil) with fluids may help control constipation.
Laxatives
If fiber doesn’t help constipation, your doctor may recommend over-the-counter laxatives, such as Milk of Magnesia or MiraLAX.
Anti-diarrheal medications
Over-the-counter medications, such as loperamide (Imodium A-D), can help control diarrhea. Your doctor might also prescribe a bile acid binder, such as cholestyramine (Prevalite), colestipol (Colestid) or colesevelam (Welchol). Bile acid binders can cause bloating.
Anticholinergic medications
Medications such as Bentyl can help relieve painful bowel spasms. They are sometimes prescribed for people who have bouts of diarrhea. These medications can cause constipation, dry mouth and blurred vision.
Tricyclic antidepressants
This type of medication can help relieve depression as well as inhibit the activity of neurons that control the intestines to help reduce pain. Side effects can include drowsiness, blurred vision, dizziness and dry mouth
SSRI antidepressants
Selective serotonin reuptake inhibitor (SSRI) antidepressants, such as fluoxetine (Prozac, Sarafem) or paroxetine (Paxil), may help if you are depressed and have pain and constipation.
Schedule An Appointment with our Naperville Functional Medicine IBS Specialist
I hope you found this article helpful. My purpose is to provide you with a different view on how functional bowel disorders occur and what might be causing them. There is a lot of information out there today on IBS and it can be confusing. Hopefully you have a little more certainty and less confusion regarding this subject. Again, it is a functional bowel disorder and for that reason I recommend a functional medicine approach. Looking for more information on our functional medicine doctor in Chicago? Contact us today!
Functional medicine strives to comprehend bodily functions, thoroughly investigate health issues, interpret findings accurately, and formulate strategies to address underlying causes of health problems. Wishing you robust health, boundless happiness, and an enriched quality of life!
Empower yourself by conducting thorough research, staying informed, and asking probing questions. Exercise discernment in evaluating the credibility of your information sources. In the healthcare sphere today, misinformation, outdated content, profit-driven interests, and biases can be pervasive, even among well-regarded sources and organizations.
This healthcare approach does not diagnose, treat, cure, mitigate, or prevent any disease. The article is provided for informational purposes only and does not replace professional healthcare services. For more information, please reach out to our office..
